VFlutter
Flight Nurse
- 3,728
- 1,264
- 113
A 84 y/o male patient presents to a rural ER after an outpatient endoscopy the previous day with complaints of shortness of breath and fatigue/malaise. Initial chest x-ray reveals infiltrates, questionable aspiration. While obtaining labs the patient begins to c/o substernal chest pain then develops hypotension. Initial cardiac enzymes negative and 12 lead shows possible ischemic changes but no definitive STEMI. Patient has history of CAD and prior MI with a stent a couple years ago. On Plavix/ASA which was held 3 days prior to procedure. Patient is placed on Dopamine drip and transferred by ground, 1hr drive, to your ICU.
Upon arrival patient is clearly in shock, mottled, and in respiratory distress. Levophed is initiated and dopamine weaned off. Patient is intubated. After intubation patient has increasing pressor requirements and worsening acidosis despite multiple liters of fluid boluses. The decision is made to place a Swan.
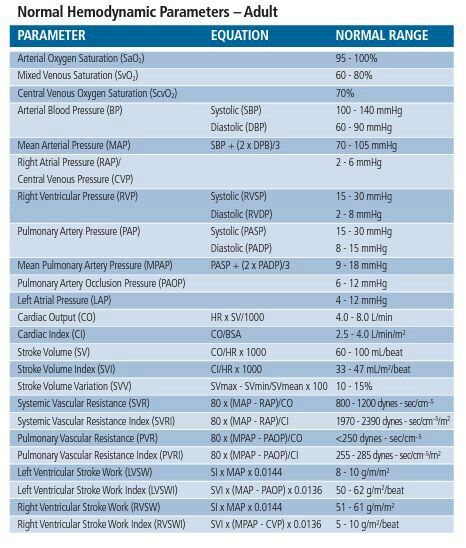
Below is the hemodynamic review for the next day. Listed at the bottom are the current drips. The blood pressures are retrieved from the latest NIBP, so they are just a snap shot in time. The patient had an arterial line and the average pressures were a little lower.
1. Differentiate the type of shock
2. Comment on the medical treatment. What was beneficial, what was not, what else could have been done.
3. Explain the pathophysiology and pharmacology of what is going on.
4. What would you anticipate for this patient? Anything you want to see done?

Levo = Levophed. Dbx = Dobutrex. Hydral = Hydralazine IV push.
Upon arrival patient is clearly in shock, mottled, and in respiratory distress. Levophed is initiated and dopamine weaned off. Patient is intubated. After intubation patient has increasing pressor requirements and worsening acidosis despite multiple liters of fluid boluses. The decision is made to place a Swan.
Below is the hemodynamic review for the next day. Listed at the bottom are the current drips. The blood pressures are retrieved from the latest NIBP, so they are just a snap shot in time. The patient had an arterial line and the average pressures were a little lower.
1. Differentiate the type of shock
2. Comment on the medical treatment. What was beneficial, what was not, what else could have been done.
3. Explain the pathophysiology and pharmacology of what is going on.
4. What would you anticipate for this patient? Anything you want to see done?

Levo = Levophed. Dbx = Dobutrex. Hydral = Hydralazine IV push.

