- 7,853
- 2,808
- 113
You're called to a pediatrician's office for a 3yo male "sick person, possible flu."
You find your patient in an exam room, seated with no assistance on the table. He tracks you as you walk in and interacts appropriately. You note his skin to be quite pale and he is on a simple mask at 4lpm. Though he appears tired, he still has normal strength throughout all extremities. Mom reports that she brought him today for flu like symptoms that have been going on for four days. Symptoms include a fever of 101.7, chills, and a productive cough. Mom reports that sometimes his coughs "sound just like a seal" but that this has not happened in several hours. Mom also relates some diarrhea over the past several days. She denies any medical history for the patient and states that she has been giving tylenol as directed for fever.
Out in the hall, you have a conversation with the pediatrician who reports that rapid flu and strep are both negative. She tells you that the patient was lethargic on arrival and hypoxic on arrival at 85% with increased work of breathing. With oxygen, the patient is satting at 95% with a good pleth and has only a minimal increase in work of breathing, his mentation has also improved. The doctor would like the patient transported to the local children's hospital, which is about 25 minutes away and also your closest facility. They are not able to acquire any lab work for you, though the doc states she is "concerned about leukemia."
Your assessment reveals the following:
Mental Status: Alert/Oriented, interacting in an age appropriate manner.
Skin: Pale, warm, dry.
HEENT: Pupils equal/round/reactive. Atraumatic. Neck supple.
Chest: Equal rise and fall bilaterally. Minor accessory muscle use noted. Rhonchus lung sounds noted in BL lower fields.
Abdomen: Soft, non-tender, non-distended.
Pelvis: Stable, non-incontinent.
Extremities: Good distal perfusion x4.
Neuro: No apparent deficits.
No signs of non-accidental trauma or anything like that. Mom is there and is very helpful with history questions. The patient appears well nourished and cared for.
Vital Signs:
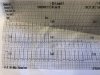
HR: 245. You think you can feel a brachial and carotid but you can't count. Strip is below.
RR: 24, moderately labored.
BP: 90/40 (manual).
SpO2: 95% @ 4lpm
Temp: 101.7 temporal
Given that mom is there, you attempt IV access with her help in the office. Following two attempts for 24ga catheters in the hand and foot, you are not able to obtain an IV. There might be an EJ you can access with a 22 but the patient is quite difficult to keep still.
So now what? What's your treatment plan? How will you transport?
You find your patient in an exam room, seated with no assistance on the table. He tracks you as you walk in and interacts appropriately. You note his skin to be quite pale and he is on a simple mask at 4lpm. Though he appears tired, he still has normal strength throughout all extremities. Mom reports that she brought him today for flu like symptoms that have been going on for four days. Symptoms include a fever of 101.7, chills, and a productive cough. Mom reports that sometimes his coughs "sound just like a seal" but that this has not happened in several hours. Mom also relates some diarrhea over the past several days. She denies any medical history for the patient and states that she has been giving tylenol as directed for fever.
Out in the hall, you have a conversation with the pediatrician who reports that rapid flu and strep are both negative. She tells you that the patient was lethargic on arrival and hypoxic on arrival at 85% with increased work of breathing. With oxygen, the patient is satting at 95% with a good pleth and has only a minimal increase in work of breathing, his mentation has also improved. The doctor would like the patient transported to the local children's hospital, which is about 25 minutes away and also your closest facility. They are not able to acquire any lab work for you, though the doc states she is "concerned about leukemia."
Your assessment reveals the following:
Mental Status: Alert/Oriented, interacting in an age appropriate manner.
Skin: Pale, warm, dry.
HEENT: Pupils equal/round/reactive. Atraumatic. Neck supple.
Chest: Equal rise and fall bilaterally. Minor accessory muscle use noted. Rhonchus lung sounds noted in BL lower fields.
Abdomen: Soft, non-tender, non-distended.
Pelvis: Stable, non-incontinent.
Extremities: Good distal perfusion x4.
Neuro: No apparent deficits.
No signs of non-accidental trauma or anything like that. Mom is there and is very helpful with history questions. The patient appears well nourished and cared for.
Vital Signs:
HR: 245. You think you can feel a brachial and carotid but you can't count. Strip is below.
RR: 24, moderately labored.
BP: 90/40 (manual).
SpO2: 95% @ 4lpm
Temp: 101.7 temporal
Given that mom is there, you attempt IV access with her help in the office. Following two attempts for 24ga catheters in the hand and foot, you are not able to obtain an IV. There might be an EJ you can access with a 22 but the patient is quite difficult to keep still.
So now what? What's your treatment plan? How will you transport?